Fentanyl binds to your opioid receptors, suppressing your breathing and causing respiratory failure, while xylazine targets your alpha-2 adrenergic receptors, dangerously lowering your heart rate and blood pressure. Because they act on completely different pathways, naloxone can reverse fentanyl‘s effects but won’t counteract xylazine’s sedation, making “tranq-dope” overdoses especially deadly. Xylazine also causes severe skin ulcers and tissue necrosis that fentanyl doesn’t. Understanding how these substances interact can help you recognize the full scope of their dangers.
What Are Xylazine and Fentanyl?

Xylazine and fentanyl are two chemically distinct substances that have become closely linked in the illicit drug supply. Fentanyl is a powerful synthetic opioid that binds to opioid receptors, producing euphoria and dangerous respiratory depression. It’s the primary driver of overdose deaths across the United States, reflecting current trends in substance abuse.
Xylazine, by contrast, isn’t an opioid at all. The FDA approved it in 1972 strictly for veterinary use as a sedative, analgesic, and muscle relaxant. It acts on alpha-2 adrenergic receptors, decreasing norepinephrine and dopamine release rather than targeting opioid pathways. You may hear it called “tranq” or “tranq dope” on the street. Understanding these pharmacological differences matters because naloxone can reverse fentanyl’s effects but won’t counteract xylazine’s central nervous system depression, highlighting nitazene class opioids. Repeated xylazine use can also cause painful skin and muscle sores that may become severe enough to require amputation. Because xylazine can dangerously slow heart rate and blood pressure, combining it with other depressants significantly compounds the threat to life.
How Xylazine and Fentanyl Attack the Body Differently
When you understand how xylazine and fentanyl attack your body, you’ll see why one drug’s antidote can’t protect you from both. Fentanyl binds to your mu opioid receptors, meaning naloxone can reverse its effects, while xylazine targets alpha-2 adrenergic receptors through an entirely different pathway that currently has no approved reversal agent. Beyond these contrasting mechanisms, each substance inflicts distinct physical damage, fentanyl drives rapid respiratory failure, whereas xylazine uniquely causes severe skin wounds, tissue necrosis, and cardiovascular collapse that won’t respond to standard opioid overdose treatment. Research comparing xylazine and lofexidine in rats has found that body weight loss during fentanyl cessation correlates with the severity of withdrawal symptoms experienced.
Different Receptor Targets
How exactly do xylazine and fentanyl differ at the molecular level? When you compare xylazine vs fentanyl, their different receptor targets explain why this synthetic opioid vs veterinary sedative pairing creates such distinct risks. Fentanyl binds primarily to µ opioid receptors, driving analgesia and respiratory depression. It also shows limited α2B adrenergic receptor interaction, though its signaling role there remains unclear.
Xylazine takes a fundamentally different path, highlighting how does xylazine work. It nonselectively binds all four α2 adrenergic receptor subtypes as a weak agonist while simultaneously activating kappa opioid receptors. You won’t find xylazine strongly engaging µ opioid receptors, and fentanyl lacks broad α2 subtype agonism. This receptor divergence matters clinically because α2A adrenergic receptors prove critical for the interactive effects when both substances are present simultaneously.
Contrasting Reversal Options
Because naloxone targets opioid receptors specifically, it fully reverses fentanyl-induced respiratory depression at effective doses (3 mg/kg in mouse models) but can’t touch xylazine’s sedative grip on the body. Xylazine symptoms, depressed breathing, low heart rate, dropping blood pressure, persist after naloxone administration. This gap defines the core danger of the fentanyl xylazine drug combination.
You should still administer naloxone if you suspect xylazine overdose risks, since fentanyl adulterants drug supply contamination means opioids are likely present. However, you’ll need to call 911 and provide rescue breaths because xylazine’s effects continue post-reversal. Researchers are exploring atipamezole alongside naloxone to address xylazine’s alpha-2 adrenergic activity, though human applications remain unestablished. Yohimbine, another alpha-2 antagonist, failed to reduce fentanyl-xylazine lethality in mouse studies at tested doses.
Distinct Physical Damage
Naloxone’s inability to reverse xylazine’s effects isn’t the only clinical gap separating these two substances, they also inflict fundamentally different types of physical harm. While fentanyl targets your respiratory system through mu-opioid receptor agonism, xylazine attacks your body’s soft tissue directly, causing wounds that don’t follow typical injection-site patterns.
If you’re exposed to xylazine-adulterated drugs, you should understand these distinct damage profiles:
- Xylazine causes severe skin ulcers and necrosis that resist standard wound healing protocols
- Fentanyl lacks association with characteristic skin ulceration seen in xylazine exposure
- Prolonged xylazine-induced immobility creates compression wounds from sustained pressure on tissue
- Necrotic lesions from xylazine may require amputation in severe, treatment-resistant cases
- Deep, unexpected skin damage signals xylazine contamination in your drug supply
Why Mixing Xylazine and Fentanyl Is So Deadly
When xylazine and fentanyl enter the body together, they attack the central nervous system through two distinct but overlapping pathways. Fentanyl binds to opioid receptors, suppressing your breathing. Xylazine simultaneously slows your brain function, heart rate, and blood pressure through a non-opioid mechanism. This dual assault compounds respiratory depression and can cause you to stop breathing entirely.
The combination creates a critical treatment gap. Naloxone reverses fentanyl’s effects but can’t counteract xylazine’s sedation. You may still experience dangerous respiratory depression even after receiving naloxone, requiring rescue breaths and continued medical intervention.
Approximately 23% of fentanyl powder seized by the DEA in 2022 contained xylazine, yet many people encounter it as an unwanted additive, meaning you may face these compounded risks without knowing xylazine is present.
How “Tranq-Dope” Entered the US Drug Supply

Before xylazine became a nationwide crisis, it had already established itself in Puerto Rico’s drug supply roughly 20 years ago, where users called it “anestesia de caballo”, horse anesthetic. By 2006, it surfaced in Philadelphia’s opioid supply, where it gained traction as “tranq dope” by the mid-2010s.
Xylazine quietly rooted itself in Puerto Rico’s drug supply before spreading to Philadelphia and eventually the entire nation.
Key milestones you should understand:
- 2006: First detected in Philadelphia overdose reports, linked to Puerto Rico’s established adulteration model
- Mid-2010s: Users actively sought xylazine-laced fentanyl for its prolonged high, boosting street demand
- 2020: Present in 25.8% of Philadelphia’s overdose deaths
- 2022: DEA seized xylazine-positive samples in 48 of 50 states
- April 2023: The White House designated fentanyl-xylazine combinations as an emerging threat
This timeline shows you how rapidly a regional adulterant became a national public health emergency.
Why Naloxone Can’t Reverse a Tranq-Dope Overdose
Although naloxone remains the frontline reversal agent for opioid overdoses, it works exclusively on opioid receptors, meaning it can’t touch xylazine’s sedative effects. When you’re facing a tranq-dope overdose, naloxone reverses fentanyl’s impact but leaves xylazine-driven respiratory depression, hypotension, and sedation fully intact.
| Factor | Fentanyl | Xylazine |
|---|---|---|
| Naloxone Response | Reversed | Unaffected |
| Respiratory Depression | Resolves with naloxone | Persists up to 20 minutes |
| Mechanism | Opioid receptor binding | Non-opioid CNS sedation |
You should still administer naloxone first, then call 911 immediately. Initiate rescue breathing to prevent hypoxic brain injury while xylazine’s effects linger. Don’t leave the person unattended, consciousness loss can recur even after an initial response. Multiple naloxone doses alongside continuous monitoring remain essential.
Why Xylazine Causes Severe Wounds and Necrosis
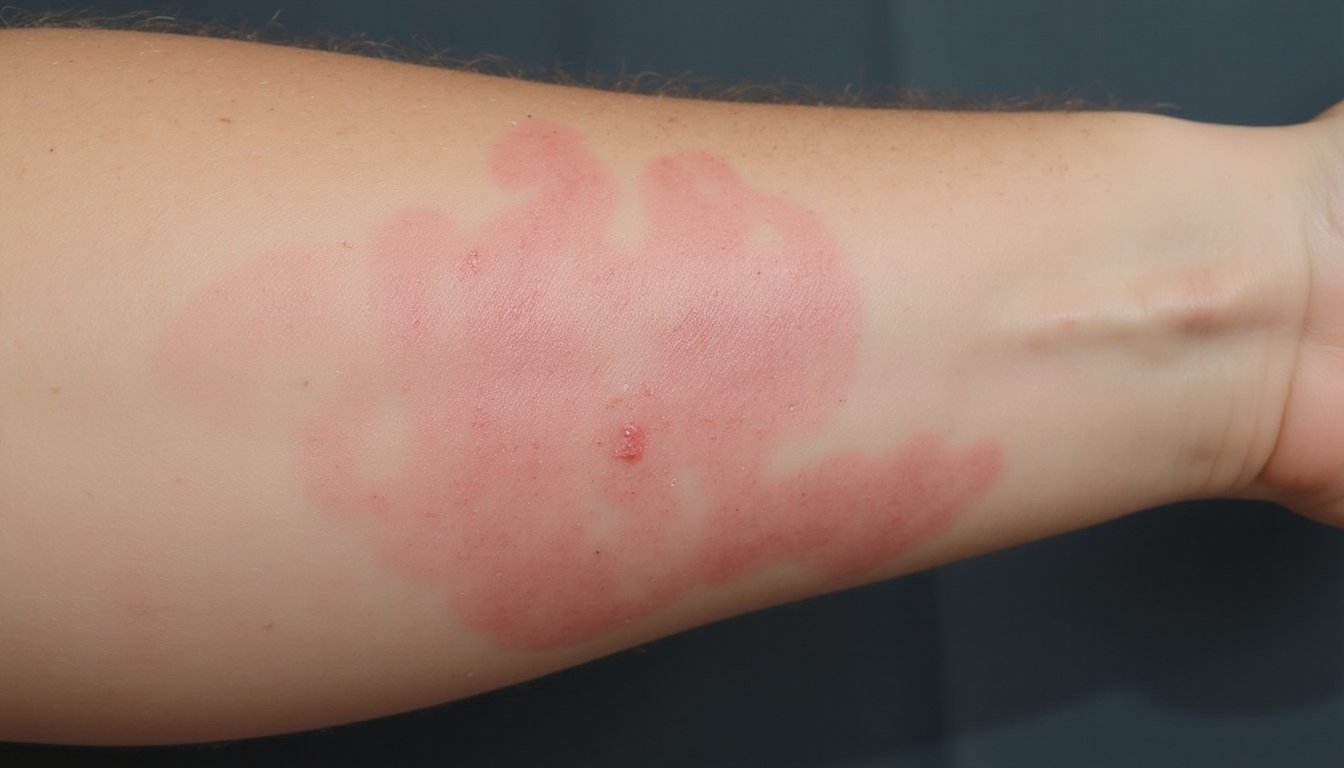
Because xylazine activates peripheral alpha-2 adrenergic receptors, it triggers intense vasoconstriction that starves surrounding tissue of oxygen and blood flow. This ischemia leads to skin necrosis, impaired wound healing, and ulcers that can expose tendons or bone. Biopsies reveal epidermal necrosis, fibrin thrombi, and small vessel vasculopathy without true vasculitis.
Xylazine chokes off blood flow at the tissue level, triggering a cascade of ischemia, necrosis, and wounds that refuse to heal.
When you reinject into already damaged tissue, you perpetuate a destructive cycle of ischemia and necrosis that produces chronic, non-healing wounds lasting months.
- Vasoconstriction reduces perfusion at injection sites, causing tissue death
- Wound progression leads to soft tissue infections, osteomyelitis, and potential amputation
- Reinjection cycles worsen damage as painful wounds prompt further use in affected areas
- Lowered cardiac output decreases systemic oxygen delivery to skin
- Early intervention remains critical to preventing irreversible necrosis
How to Detect Xylazine and Fentanyl in Street Drugs
Given that xylazine now appears in over 80% of urine samples tested at the U.S.-Mexico border, always alongside fentanyl, detecting these substances before use has become a frontline harm reduction priority. You can use Wisebatch xylazine test strips, which detect xylazine in 82.6% of urine samples, while BTNX fentanyl strips accurately identify fentanyl at 0.125 micrograms/ml. Some manufacturers now offer 2-in-1 strips covering both substances.
However, you should know these tools have limitations. Lidocaine, present in 30.4% of samples, may interfere with xylazine strip accuracy. Mass spectrometry remains the gold standard, confirming xylazine in 52.2% and fentanyl in 73.9% of paraphernalia samples. Regardless of test results, you should always carry naloxone, which reverses opioid effects even when xylazine is present.
Why Xylazine Makes Fentanyl Withdrawal Worse
When you’re dependent on fentanyl laced with xylazine, withdrawal hits harder because xylazine activates kappa opioid receptors, intensifying symptoms beyond what fentanyl alone produces, and this intensification often arrives on a delayed timeline that catches you off guard. You’re also likely to experience greater physical weight loss during withdrawal, as the combined burden of dual-substance dependence amplifies somatic effects, particularly in females. Perhaps most critically, there’s no reversal agent that effectively targets xylazine’s withdrawal syndrome, meaning naloxone addresses the fentanyl component while leaving xylazine-driven symptoms like anxiety, dysphoria, and autonomic instability unmanaged.
Delayed Withdrawal Intensification
Though researchers once believed xylazine acted solely on α2-adrenergic receptors, recent findings reveal it also activates kappa opioid receptors, a mechanism that directly intensifies fentanyl withdrawal. When you receive naloxone during an overdose involving both substances, this dual activation triggers withdrawal that’s more severe than either drug produces alone. Female mice in preclinical studies showed synergized withdrawal responses, confirming this intensification isn’t purely additive.
This kappa opioid activity means your withdrawal timeline shifts unpredictably:
- Symptoms begin 12, 24 hours after your last dose and peak at 1, 3 days
- Xylazine-specific symptoms overlap with opioid withdrawal, complicating diagnosis
- Additional opioids won’t relieve xylazine-driven distress
- Prolonged anxiety and cravings persist weeks to months
- Uncertain drug concentrations make timing predictions unreliable
These compounded effects drive continued use to avoid increasingly aversive withdrawal.
Greater Physical Weight Loss
Because chronic co-exposure to fentanyl and xylazine produces a unique opioid-like somatic withdrawal syndrome not seen with either drug alone, your body undergoes measurably greater physical deterioration during cessation, including significant weight loss.
| Factor | Impact on Weight Loss |
|---|---|
| Xylazine dose | Higher doses intensify withdrawal severity and physical decline |
| CNS rebound | Triggers anxiety, restlessness, and metabolic stress within 6-12 hours |
| Peak withdrawal | Weight loss concentrates within 1-3 days post-cessation |
| Recovery timeline | Lingering fatigue and muscle weakness persist 1-2 weeks |
Notably, xylazine suppresses weight loss during the first 24 hours of fentanyl withdrawal, masking early deterioration. Once this suppression lifts, you’ll experience accelerated physical decline that standard opioid treatments can’t adequately address.
No Reversal Agent Available
Unlike fentanyl, which naloxone can rapidly reverse, xylazine has no FDA-approved reversal agent, and that’s what makes combined withdrawal so dangerous. When you’re experiencing a mixed overdose, naloxone addresses only the opioid component, leaving xylazine’s respiratory and cardiovascular depression unchecked.
You should understand the key clinical implications:
- Naloxone doesn’t reverse xylazine-induced bradycardia, hypotension, or respiratory depression
- No FDA-approved medications exist specifically targeting xylazine withdrawal
- Alpha-2 agonists like clonidine are used off-label to manage rebound sympathetic excitation
- Standard buprenorphine or methadone induction won’t alleviate xylazine-specific symptoms
- Conventional opioid protocols fail to account for xylazine’s independent CNS effects
This pharmacological gap means your treatment team must deploy novel, multi-drug strategies beyond traditional opioid withdrawal management.
How Communities Are Fighting Tranq-Dope Deaths
The rapid spread of xylazine-laced fentanyl, commonly called “tranq dope”, has forced communities across the country to mount urgent, multifaceted responses. In Philadelphia’s Kensington neighborhood, where tranq appears in over 90% of dope samples, nurses like Katie Mowrey and Stephanie Klipp provide direct care to tranq-dependent individuals on the streets.
In rural areas, you’ll find community-led initiatives filling critical gaps. In Greenville, NC, 77-year-old Diannee Carden founded EkiM, the only needle exchange program for hundreds of miles. Her organization delivers harm reduction education and helps users understand what substances they’re ingesting.
San Francisco’s medical leadership has called for expanded outreach and addiction treatment. Meanwhile, the White House declared fentanyl-xylazine mixtures an emerging threat in April 2023, signaling federal commitment to addressing tranq dope‘s devastating impact.
Reach Out and Take Back Control
Substance use can quietly damage your health, strain your relationships, and disrupt your daily routine, but recovery is possible with the support you need. At Simonds Recovery Centers, we offer personalized Fentanyl Addiction Recovery Programs with experienced therapists and addiction specialists ready to guide you toward healing. Call +1 (833) 781-8338 today and begin your journey to a healthier, drug-free life.
Frequently Asked Questions
Is Xylazine Classified as a Controlled Substance by the DEA?
No, xylazine isn’t currently classified as a controlled substance by the DEA at the federal level. It’s FDA-approved only for veterinary use, and it operates in a regulatory gap that allows diversion without federal controlled substance penalties. However, the DEA has initiated scheduling processes, and Congress introduced the Combating Illicit Xylazine Act in 2023. You should know that some states, like Pennsylvania, have independently scheduled xylazine.
Can Fentanyl Test Strips Also Detect Xylazine in Drug Samples?
No, fentanyl test strips can’t detect xylazine in your drug samples. They’re designed specifically to identify fentanyl and won’t cross-detect xylazine, since these substances belong to different pharmacological classes. You’ll need separate xylazine test strips, which show 100% sensitivity and 85% specificity in lab testing. You can test the same dissolved sample with both strips simultaneously, but each strip works independently. Always combine test results with other risk reduction practices.
What Animals Is Xylazine Legally Approved to Be Used On?
The FDA has approved xylazine for use on dogs, cats, horses, elk, and several deer species, including white-tailed, fallow, mule, and sika deer. You’ll also find it used off-label in cattle, sheep, rats, and mice, though these aren’t formally FDA-approved applications. Veterinarians commonly rely on xylazine for sedation, pain relief, and muscle relaxation, making it an essential tool when you’re managing both domestic and wildlife species safely.
Are There Any Medications Being Developed to Reverse Xylazine Overdose?
Currently, no approved antidote exists specifically for xylazine overdose in humans. However, researchers are exploring promising options. Atipamezole, an α2-antagonist used in veterinary medicine, has shown effectiveness in human trials for reversing xylazine’s sedative and cardiovascular effects. Yohimbine has reversed xylazine’s effects in animals but isn’t approved for you. If you’re witnessing an overdose, you should still administer naloxone, provide rescue breaths, and call 911 immediately.
How Does Xylazine Affect the Body Differently When Injected Versus Smoked?
When you inject xylazine, you’re at higher risk for severe skin wounds, necrotic tissue, and abscesses at the injection site, which can lead to amputation. It also rapidly slows your breathing, heart rate, and blood pressure. When you smoke it, you’ll still experience dangerous sedation and skin lesions, but they typically appear on your arms, legs, or feet rather than at a direct injection site, with generally less tissue destruction.





